|
To Print: Click your browser's PRINT button.
NOTE: To view the article with Web enhancements, go to: http://www.medscape.com/viewarticle/510997 Exercise as a Treatment for Osteoarthritis Kim Bennell; Rana Hinman Curr Opin Rheumatol. 2005;17(5):634-640. ©2005 Lippincott Williams & Wilkins Posted 09/08/2005 Abstract and IntroductionAbstractPurpose of Review: This review highlights recent important research, future directions, and clinical applications for exercise and osteoarthritis. It focuses on knee osteoarthritis because of its prevalence and the dearth of research involving other joint osteoarthritis. The review covers exercise prescription for symptomatic relief, and its potential role in reducing development and slowing progression of osteoarthritis. IntroductionOsteoarthritis is a chronic joint disorder with the knee most frequently affected.[1] Patients often report pain, muscle weakness, stiffness, and instability, as well as reduced physical functioning. Ultimately, these lead to a loss of independence and a reduction in quality of life. In the past, studies have evaluated the role of exercise as a tertiary prevention strategy (treating pain and disability) but more recently, its potential role in primary (reducing disease incidence) and secondary (slowing progression to serious disease) prevention is receiving increasing attention. The Purpose of this review is to highlight recent important research, future directions, and the clinical application of research findings in the area of exercise and osteoarthritis. This review focuses on knee osteoarthritis because of its prevalence[1] and the dearth of research involving hip and other joint osteoarthritis. This review will cover: exercise prescription for symptomatic relief of osteoarthritis, the role of exercise in reducing development of osteoarthritis, and the role of exercise in slowing disease progression. Exercise Prescription for Symptomatic Relief of OsteoarthritisAs there is currently no cure for osteoarthritis, most research continues to evaluate the use of exercise as a treatment to alleviate symptoms of the disease. Recent common themes in the literature will be explored in this section, and the Results of studies discussed in relation to clinical practice. Clinical Guidelines and Meta-analysesClinical guidelines have been developed by leading bodies (American College of Rheumatology and the European League Against Rheumatism) to aid health practitioners in treating osteoarthritis.[2,3] These recommend exercise therapy to reduce pain and improve function, based largely on expert opinion and the Results of large randomized controlled trials evaluating exercise.[4-6] Recent meta-analyses support these recommendations.[7-9] Two published in 2004 focus specifically on the efficacy of strengthening[8•] and aerobic exercise[9•] for osteoarthritis. Twenty-two trials of strengthening exercise were identified and included isometric, isotonic, isokinetic, concentric, concentric-eccentric, and dynamic modalities. Improvements in strength, pain, function, and quality of life were noted with muscle strengthening; however, there was no evidence that the type of strengthening exercise influences outcome. Findings suggest that the effectiveness of joint- specific strengthening is maximized when combined with general strength, flexibility, and functional exercises. Regarding aerobic exercise, 12 trials were identified including walking programs, aquatic exercises, jogging in water, yoga, and T'ai Chi. Results indicated that aerobic exercise alleviates pain and joint tenderness, and promotes functional status and respiratory capacity. While strengthening appears superior to aerobic exercise in the short-term for specific impairment-related outcomes (e.g. pain), aerobic exercise appears more effective for functional outcomes over the longer term. Different exercise types have different effects; thus, an individualized approach to exercise prescription is recommended, based on presenting symptoms, problems and the needs of the patient. Roddy et al.[10••] published evidence-based recommendations for exercise in managing hip and knee osteoarthritis. These recommendations are unique in that they combine and differentiate expert opinion and research evidence, as well as address important clinical questions such as adherence, predictors of response, need for individualized exercise prescription, and mode of exercise delivery. Recommendations include the following:
Unfortunately, many of the recommendations proposed by expert opinion have not been researched; however, they provide a valuable framework to guide clinical practice and future research directions. Developing Specific and Novel Exercise ProgramsOsteoarthritis is heterogeneous with regards to associated symptoms, impairments, and changes in the local mechanical environment.[11] This has implications for the development of novel exercise programs and for tailoring standardized programs to suit specific patient subgroups. Traditionally, exercise therapy for knee osteoarthritis has centered on quadriceps strengthening; however, it appears that such an exercise strategy may not be the optimal choice for all patients. For example, functional instability, the symptom of buckling, slipping, or giving way of the knee during functional activities, has recently been identified as a problem in a significant proportion of individuals with knee osteoarthritis. In a cohort of 105 people, 44% reported instability that affected their ability to function.[12•] Instability is likely to be multifactorial, resulting from factors such as passive joint laxity, structural damage, muscle weakness, pain, and altered neuromuscular control. Further research needs to examine the extent these factors contribute to the symptom of instability in knee osteoarthritis as this will influence treatment strategies utilized. Fitzgerald et al.[1] suggest an agility and perturbation training program may be effective by exposing the individual to potentially destabilizing loads in a controlled manner allowing the neuromuscular system to adapt to such conditions. The effect of such an exercise program requires formal evaluation before widespread implementation clinically. Muscle strengthening is a key component of exercise for osteoarthritis because of the relation between muscle weakness and pain and function.[14,15] However, traditional muscle strengthening exercises may be inadequate in the subgroup of patients whose strength loss is largely because of central-mediated or reflex-mediated inhibition.[16] Instead, more specialized interventions may be needed to supplement volitional exercise programs. Identifying muscle inhibition is currently difficult in a clinical setting; it may be worth considering other interventions if strength gains with exercise are not as great as would be expected. Evaluating the Interaction of Exercise With Other InterventionsClinical practice generally implements more than one treatment concurrently for patients with osteoarthritis. Past research has tended to evaluate exercise therapy in isolation or in combination with other treatments. However, for the latter, study design precludes the elucidation of interaction effects. It is likely that exercise, when combined with other efficacious treatments, maximizes clinical outcome. This is supported by the recent 18-month randomized, single-blind ADAPT trial.[17••] The Results in 316 overweight and obese individuals with knee osteoarthritis showed that the combination of modest dietary weight loss and moderate exercise (aerobic and strengthening exercise three times per week) provides better overall improvements in function, pain, and mobility than either intervention alone. A similar study design evaluating exercise and drug therapies in particular is required. Mode of DeliveryRising healthcare costs necessitate delivering exercise in the most cost-effective and efficacious method. A Cochrane Review compared the effect size of exercise delivered as individual treatments, supervised group classes, and home exercise.[18] For pain, comparable medium effect sizes were observed with individual treatments and group classes, while a small effect size was evident for home exercise. Small effect sizes were reported for all modes of delivery regarding physical function. This suggests that supervised group or individual treatments are superior to independent home exercise. A 'minimalist' approach to exercise intervention seems ineffective in patients with hip and knee osteoarthritis.[19•] In a large study, rheumatologists randomly delivered one of four interventions: patient-administered assessment tools, home exercise, patient-administered assessment tools plus home exercise, or usual care. The exercise program aimed to improve joint mobility and increase muscle power. The rheumatologist provided an oral explanation of the importance of exercise and a booklet illustrating the exercises as well as a videotape. There was a limited capacity to expand the exercise program. There was no difference in outcome between interventions. Numerous factors likely contribute to the ineffectiveness of exercise in this study. Patients were poorly compliant (only 29-33% met the specified criterion of adherence) and a standardized exercise program and dosage was used that may have been ineffective for such a heterogenous patient group. While a videotape demonstration of the exercises was provided, it would appear that technology is no substitute for personal demonstration and instruction in correct exercise technique. It is quite possible that many patients were performing the exercises incorrectly, further reducing their effectiveness. Others have studied the effects of supplementing home exercise with a class-based program.[20•] Patients were taught home exercises with their intensity individualized at baseline and reassessed and increased at 4-week and 8-week reviews. In addition, half of the patients were randomly allocated to undertake an 8-week physiotherapist-supervised class exercise program. Results demonstrated that supplementation of a home program with exercise classes lead to greater improvements in pain and locomotor function at 12 months follow-up. Importantly, this study demonstrates that the short-term addition of exercise classes to an ongoing home exercise program Results in significant symptomatic benefits in the longer term. Economic analyses demonstrated that the additional cost of the group exercise classes was offset by reductions in resource use elsewhere in the healthcare system.[21] Thus, exercise class supplementation represents a relatively cost-effective method of maximizing the benefits of a home exercise program that would otherwise result in only small benefits of questionable clinical effectiveness. Improving Uptake of Exercise in the Osteoarthritis PopulationDespite evidence of the benefits of exercise in osteoarthritis, the challenge remains to increase the proportion of patients exercising. While there are many barriers to the uptake of exercise in the osteoarthritis population, two are of particular importance: recommendation of exercise to patients by medical practitioners and appropriate referral to exercise professionals, and compliance by patients with prescribed exercise programs. Exercise is under-used by medical practitioners as a treatment strategy for osteoarthritis. A French study surveyed 3,000 general practitioners as to their treatment of a hypothetical knee osteoarthritis patient..[22•] Less than 15% of general practitioners reported that they would prescribe exercise as a first-line therapeutic approach. Perhaps even more alarming is the finding that bed rest was recommended (2% of general practitioners for less severe osteoarthritis and 24% for more severe disease), despite the lack of evidence for this outdated treatment method. A survey of osteoarthritis patients in Canada revealed that only one-third had been advised to use exercise for their condition;[23] however, 73% reported that they had tried exercise in the past. Given the large number of patients who chose to try exercise independently, it is possible that many failed to consult a professional regarding the most appropriate exercise to commence. Thus, it is likely that many patients selected inappropriate exercise programs or dosages. Coupled with the risk of incorrect technique, many patients may have failed to achieve any therapeutic benefit from exercise. Patient compliance is a key factor in determining outcome from exercise therapy in osteoarthritis patients. Ettinger et al.[] demonstrated a dose-response relation between compliance and exercise effects. The strongest and most consistent predictor of compliance in this study was exercise behavior in the previous months of the trial,[24] suggesting that the 'habit' of exercise is important in determining future exercise behavior. Similarly, effect sizes with home exercise drop from medium to small as self-reported adherence falls.[25] Unfortunately, the beneficial effects of exercise in osteoarthritis last only as long as the patient exercises, as demonstrated in a follow-up of 183 patients 6 months after completion of a 12-week exercise program.[26] Although exercise resulted in significant improvements in pain and disability, these effects were lost 6 months after the exercise program had ceased. Another study evaluated the factors that motivate patients with knee osteoarthritis to join a 12-month trial comparing strength training and flexibility exercise.[27] Results indicated that social support, the presentation of an organized exercise opportunity conducted by professionals, having a partner exercise alongside the patient, familiarity with the exercise task, and having positive outcome expectations of exercise were all important. Campbell et al.[2] interviewed knee osteoarthritis patients who had participated in a physiotherapy trial consisting largely of home-based strengthening exercises. Patients were most compliant in the initial period while still seeing the physiotherapist. However, compliance declined once therapist contact ceased. Reasons cited as affecting motivation to comply included attitude towards exercise, perceived severity of symptoms (those with more severe symptoms were most likely to comply), ideas about the cause of arthritis (those who thought arthritis was the result of age or 'wear and tear' were less compliant) and the perceived effectiveness of the intervention (high levels of continued compliance were related to the perception that physiotherapy is effective and an improvement in symptoms was experienced). The Role of Exercise in Preventing Disease DevelopmentWhether exercise can prevent osteoarthritis is unclear but from a public health perspective, primary prevention is an area worthy of investigation. It is thought that contraction of the quadriceps muscle helps to absorb shock at heel strike.[29] A direct link between impact loading and development of osteoarthritis has only been shown in animal models.[30,31] A potential relation between muscle strength and disease development was first reported by Slemenda et al.[3] who found that in women, but not men, stronger quadriceps muscles reduced the risk of developing radiographic knee osteoarthritis. Two recent studies support these Results. Hootman et al.[33•] evaluated 3081 community-dwelling adults free of osteoarthritis, joint symptoms, and injuries. Women with a moderate to high isokinetic quadriceps strength had a 55% and 64% reduced risk of developing hip or knee osteoarthritis, respectively. The Results were less conclusive for men. The relationships between body composition measured using dual energy x-ray absorptiometry, and changes in tibial cartilage volume over 2 years were measured by magnetic resonance imaging (MRI) in 86 healthy middle-aged adults.[34] Increased muscle mass was strongly associated with medial tibial cartilage volume as well as a reduction in the loss of both medial and lateral tibial cartilage volume. Body fat was not an independent risk factor for cartilage loss. These Results are consistent with another study also showing a positive association between muscle size and knee- cartilage volume.[35] However, co-inheritance rather than local muscle hypertrophy arising from exercise, may explain these relationships. In fact, a common genetic link for these parameters was established in a recent sib-pair study.[36] Furthermore, in the study by Cicuttini et al.[3] the relation between tibial cartilage volume and muscle mass was significant for multiple sites (the lower limbs, all four limbs, and total body muscle mass) rather than being isolated to a particular limb that would support a co-inherited mechanism. Randomized controlled trials are needed to establish whether exercise interventions designed to increase muscle mass do, in fact, protect against future hip and knee osteoarthritis. Role of Exercise in Slowing Disease ProgressionKnee load plays a role in disease progression. The external knee adduction moment generated during walking forces the knee laterally into varus, compressing the medial joint compartment. It is one of a few factors known to predict progression of osteoarthritis in humans.[37] Therapeutic exercise could have a disease-modifying effect by altering knee joint load but whether this effect is positive or negative is unclear as only indirect evidence exists. A potential effect of strengthening exercise on disease progression was first explored in 1999. However, this longitudinal cohort study failed to find a relation between quadriceps strength and disease progression possibly because of limited statistical power.[38] Controversy was later triggered by the unexpected Results of another study[3] where higher baseline quadriceps strength was associated with a greater risk of disease progression in knee osteoarthritis patients with malalignment and laxity. In neutrally aligned and stable knees, there was no relation between strength and progression. This suggests that exercise may have differential effects depending on patient presentation and highlights the need for specificity of exercise prescription. Though the focus has been on quadriceps strength, it may be that other muscles also influence knee load and hence disease progression. During walking, the abductor and adductor muscles stabilize the pelvis on the hip joint and thus weakness may influence pelvic level or toe out angle during gait thereby increasing the knee adduction moment.[40] An abstract of a longitudinal cohort study found that those with a lower external hip adduction moment (indicating less use of the hip abductor muscles) had more rapid knee osteoarthritis progression.[41] Greater toe out is associated with a lower adduction moment and reduces the odds of radiographic progression.[42] Less is known about the hip adductor muscles in relation to knee osteoarthritis but they may assist in resisting the knee AM, particularly in a varus malaligned knee. By virtue of their attachment to the distal medial femoral condyle, the adductors could eccentrically restrain the tendency of the femur to move into further varus. Yamada et al.[4] found that patients with knee osteoarthritis had stronger hip adductors compared with age-matched controls, and that those with more-severe osteoarthritis had even stronger adductors than their less-severe counterparts. They hypothesized that this increased strength may be because greater use of the hip adductors in an attempt to lower the knee adduction moment. Given that hip mechanics can alter knee load, hip strengthening could be a novel intervention for rehabilitation of knee osteoarthritis patients. This requires further evaluation. Reductions in muscle strength and proprioception, and abnormal gait patterns are well described in knee osteoarthritis.[44-46] However, there is growing recognition that other aspects of neuromuscular control, such as muscle activation strategies, are also altered. Recent cross-sectional electromyographic studies have identified differences in both the timing and amplitude of muscle activity in patients with knee osteoarthritis compared with healthy controls.[47•,48,49••,50•] Childs et al.[4] found that the lower limb muscles were activated for 1.5 times longer in osteoarthritis compared with controls during walking and stair ascent and descent. Greater muscle co-activation between the vastus lateralis and the medial hamstrings was also evident in the osteoarthritis group. Others have similarly reported increased levels of co-contraction with greater activation of the hamstrings.[49,50] Lewek et al.[4] reported that differences in co-contraction levels comparing osteoarthritis patients and controls were confined to the medial side with similarly high levels of lateral muscle co-contraction in the two groups. This was associated with greater medial joint laxity, a higher adduction moment and more self-reported instability in the osteoarthritis group compared with controls. The authors suggest that frontal plane laxity is localized to the medial side of the joint in osteoarthritis and that the greater medial co-contraction is an attempt at stabilization. However, this strategy is likely to result in greater medial joint compressive loads and thus may hasten disease progression. These neuromuscular alterations in knee osteoarthritis represent coping strategies to combat pain, weakness, or local mechanical changes including joint laxity. While such strategies may have short-term benefits, they may have long-term negative consequences by altering the distribution and increasing the magnitude of load and potentially speeding disease progression. This has led to the recommendation that novel exercise approaches designed to reduce levels of co-contraction should be developed to address these neuromuscular changes.[47•,50•] Further research is needed to identify the patient subgroups most likely to present with these changes, how these changes can be identified in the clinical setting, and to develop and test novel interventions. ConclusionTo maximize overall patient outcome, an exercise program incorporating strengthening and aerobic elements together with other specific exercises based on individual requirements is most appropriate. In the future, it is likely that novel exercise regimes will be developed to address recently identified neuromuscular changes and impairments associated with osteoarthritis and having the potential to influence disease progression. Maximizing compliance is a key element dictating success of exercise therapy. This could be enhanced by the use of supervised exercise sessions (possibly in class format) in the initial exercise period to allow appropriate patient education regarding benefits of exercise, ensure safe and correct exercise technique, and provide a supportive social environment for exercise (Fig. 1). At this early stage, prescription and instruction in tailored home exercises by a suitably trained professional is also important. Bringing patients back for intermittent consultations with the exercise practitioner, or attendance at 'refresher' group exercise classes may assist long-term compliance. 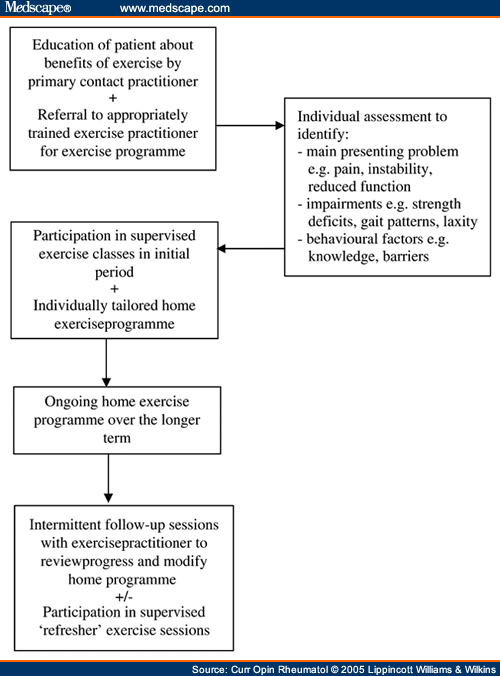 Figure 1. References Papers of particular interest, published within the annual period of review, have been highlighted as:
Reprint Address Associate Professor Kim Bennell, Centre for Health, Exercise and Sports Medicine, School of Physiotherapy, University of Melbourne, Melbourne, Australia 3050, Tel: +61 3 83444171; fax: +61 3 83444188; e-mail: k.bennell@unimelb.edu.au Kim Bennell, Rana Hinman, Centre for Health, Exercise and Sports Medicine, School of Physiotherapy, University of Melbourne, Melbourne, Australia |